Article Text
Abstract
Background The contraceptive prevalence rate in Mozambique was estimated as 11.3% in the last Demographic and Health Survey. The impact of family planning (FP) on women's health and on the reduction of maternal mortality is well known.
Methods Acknowledging the importance of user satisfaction in the utilisation of health services, exit interviews were used to assess women's satisfaction with FP services in Mozambique. The survey, conducted in 174 health facilities, was representative at the national level, covered all provinces, and both urban and rural areas.
Results Overall, 86% of respondents were satisfied with FP services, but issues such as insufficient supplies of oral contraceptives and the low quality of healthcare provider/client interactions were given as reasons for women's dissatisfaction.
Conclusion Defined actions at the level of health service provision are needed to tackle the identified issues and ensure improved satisfaction with, and better utilisation of, FP services in Mozambique.
- family planning service provision
- patient satisfaction
- Mozambique
This is an Open Access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/
Statistics from Altmetric.com
Key message points
Overall there is a high level of satisfaction among women attending family planning (FP) services in Mozambique.
Insufficient supplies of contraceptives, long waiting times, and poor provider/client interactions are all factors that adversely impact on women's satisfaction with FP services.
Healthcare providers are the primary source of information about contraceptive methods and their benefits for women attending FP services.
Women's satisfaction with FP services can be increased by improving supplies of oral contraceptives, identifying strategies for reducing waiting times, and improving the quality of provider/client interactions.
Introduction
Maternal mortality represents an important worldwide public health topic. The United Nations estimates that approximately 303 000 maternal deaths occurred globally in 2015, corresponding to a maternal mortality ratio (MMR) of 216 per 100 000 live births.1 Although this ratio represents a 43% decrease in MMR since 1990, the number of deaths is still quite high. From the 2013 World Health Organization estimation, for Mozambique, the estimated MMR was more than twice the global level at 480/100 000 live births.2 It has been shown that family planning (FP) positively contributes to the reduction of maternal deaths. It has been estimated that the uptake of contraception in countries with high birth rates has the potential to prevent up to 32% of maternal deaths and nearly 10% of infant deaths.3 Other authors have estimated a 29% reduction in maternal deaths per year if the unmet need for FP is satisfied.4One of the main contributions of the International Conference on Population and Development held in Cairo in 1994 was the recognition that satisfaction of sexual and reproductive rights is a human rights issue.5 This conference led to a global effort to recognise the importance of FP within maternal and child health programmes as a mechanism to improve the accessibility and availability of modern contraceptive methods. Despite these efforts, the use of modern methods as measured by the contraceptive prevalence rate (CPR) remains low in many developing countries, with a growth of 1% per year, over the last 30 years.6 Mozambique is a sub-Saharan country with an estimated CPR of 11.3% among married women and a total fertility rate of 5.9.7 Mozambique had the lowest CPR when compared to neighbouring countries.8 Unpublished administrative data from the Ministry of Health indicates that from 2009 to 2011 the use of contraceptive methods (measured by the number of new users) increased. However, a stable but low CPR might also be indicative of discontinuation in method use.9
One of the factors that influences the use of FP and other reproductive health services is client satisfaction with healthcare services.10 Users’ satisfaction has been studied extensively at the global level and a number of determinants, including accessibility to health services, continuity of care, consultation time, waiting time, and provider/client relationship, have been identified as key factors correlated with satisfaction levels.11 In Mozambique no recent studies on service satisfaction could be found; however, research completed in other areas of sub-Saharan Africa confirms the importance of waiting time, friendliness of staff, women's education, and distance/proximity to health facilities as the main determinants of client satisfaction.12–14
The aim of this study was to assess the satisfaction and associated factors among women attending FP services at public health facilities in Mozambique.
Methods
Study setting
This study was conducted in public primary level health facilities in both urban and rural areas across 11 provinces throughout the country. In 2011, Mozambique had a total of 1386 healthcare facilities, of which 1338 offered FP services on a regular basis.
Sampling the health facilities
The sample of health facilities was drawn from all facilities that routinely offered FP services. A representative sample was selected, stratified by province and type of health facility. The health facilities were divided into four groups: ‘Class 1’ – District Hospitals, ‘Class 2’ – Health Centers Type I, ‘Class 3’ – Health Centers Type II and ‘Class 4’ – Health Posts. Of the total eligible health facilities, all 23 facilities from Class I were included and 151 facilities were selected from the remaining 1315 facilities, producing a final sample size of 174 health facilities. According to the relative weighting of the different types of health facilities providing FP services in each province, the total sample size was proportionally allocated in each of the 11 provinces. Class 2, 3 and 4 health facilities were randomly selected within each province.
Sampling the women to be interviewed
Women were sampled by selecting users who had left or were about to leave the FP service site on the interview day. The estimated number of women selected and interviewed in each facility was calculated according to the average number of clients seen in the last 7 days. The women to be interviewed were selected systematically by selecting every mth woman who was about to leave the FP services, where ‘m’ was based on the average number of consultations per day over the previous 7 days.
Data collection
A questionnaire was adapted from one used by the United Nations Population Fund and pre-tested locally. Data collectors were selected from maternal and child health nurses and trained in the use of the tool and data collection techniques. The data collection occurred in December 2011.
A database was created using the Statistical Package for the Social Sciences (SPSS) V.17.0 (SPSS Inc., Chicago, IL, USA); this software was used for data entry. Ethical approval for the study was granted by the National Health Ethical Committee of Mozambique.
Measurement of satisfaction
To measure women's satisfaction a composite variable ‘general satisfaction’, with an ordinal scale, was constructed by summing the ratings of the following three questions: (1) Did the woman feel well treated by the health provider? (2) Was the woman satisfied with the overall services and care in this health facility? (3) In the woman's opinion, besides the nurse or doctor, did the other staff treat her well? These questions were rated as follows: −1 if No, 0 if failed to answer, and 1 if Yes. If the sum resulted in a negative value, then the user was considered to be ‘dissatisfied’ (No), between 0 and 1 as ‘somewhat satisfied’ and above 1 as ‘satisfied’ (Yes).
Satisfaction was then analysed against the client and facility factors such as type of healthcare facility, the woman's age, quality of provider/client interaction, user's occupation, access to information on FP, duration of using contraceptive method, and waiting time at the health facility. The quality of provider/client interaction was a composite variable obtained by summing 10 different questions which were all binary coded. The resulting values were categorised into low (0–3), medium (4–6) and high quality of interaction (7–10) based on the number of positive answers.
Statistical methods
Although ordinary baseline logistic models can be applied to an analysis of the probability of categorical outcomes, they are not appropriate for ordinal outcomes such as satisfaction since they ignore the natural order of the categories or levels of the variable, resulting in a considerable loss of statistical power. Walker and Duncan,15 and later McCullagh,16 proposed the use of proportional odds models for the analysis of ordinal outcomes.
A multiple logistic regression using a proportional odds assumption was applied to assess the effect of the covariates on general satisfaction (Table 3). Probabilities were summed from No to Yes across the satisfaction scale. We tested the proportional odds assumption using a Score test, which failed to reject it at the 5% significance level.
In this model, cumulative probabilities are expressed as functions of the explanatory variables. One key assumption of this model is that the regression coefficients or odds ratios (ORs) are identical for each of the k (k=1, 2, 3) cumulative probabilities, hence the name ‘proportional odds model’. The model for the kth category can be expressed as follows, for k=1, 2,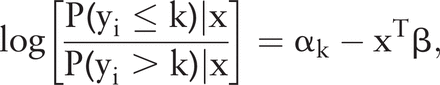
where y represents the outcome variable (satisfaction) with three levels; αk represents the intercept term, which is ordered to reflect the order of the cumulative probabilities, x is a matrix containing the covariates or factors, and β is a parameter vector containing regression coefficients associated with the covariates in x. In this model, an OR can be obtained by exponentiation of the estimates in the vector β. This model was fitted using Statistical Analysis System (SAS) V.9.2.
Results
The findings are divided into different themes such as general characteristics of the women, utilisation of FP services, client access to information on FP, the provider/client interactions, waiting time, and user satisfaction.
Of the 174 sampled health facilities, the study was conducted in 149 (85%) representing all provinces, and both urban and rural areas. Three (13%) District Hospitals, 6% of the Type II Health Centers and 16 (45%) Health Posts were excluded from the study due to a lack of FP services being offered on the day of the interview, and/or in some cases due to them being geographically inaccessible.
A total of 671 women were included in the sample, of which 18% were interviewed at District Hospitals, 54.5% at Type II Health Centers, 14.6% at Type I Health Centers and 12.8% at Health Posts.
Around 42% of the interviewees were aged between 21 and 30 years (average age 28 years). The majority (76.6%) of women lived with a partner. The majority (57.7%) of the women worked in subsistence agriculture, 17.6% were housewives and 11.3% were students. Around 82% of the women had walked to the nearest FP services, taking on average 58 minutes to reach the clinic.
Utilisation of FP services
Regarding the reasons for using FP, 76.5% of the women said that they wanted to space their pregnancies, 13.5% said that they were no longer interested in becoming pregnant, and 8.3% reported that they were at high obstetric risk. On the interview day, 62.7% of women said that they had come for a follow-up consultation, 32.3% were having their first FP consultation that day, and 3.4% were attending for postpartum contraception.
The oral contraceptive pill was the most commonly requested FP method (52.2%), followed by injectable contraception (41.6%) and the lactational amenorrhea method (4.3%). Only three (<0.5%) women reported using the intrauterine device (IUD). On average, women said that they had been using their current FP method for 5 months and 3 weeks, while 24.1% reported that they had changed their method (once) in the last 5 months. The main reasons for changing method were: (1) spotting reported by 36.4% of pill users and 27.4% of injectable contraception users and (2) the lack of contraceptive methods at the health facility on the day of their visit, a factor that was mentioned by 11.4% of pill users and 27.4% of injectable contraception users. On average, pill users received 1.2 blister packs at each consultation and 38.2% were not satisfied with this quantity of contraceptives.
Access to FP information
Healthcare providers were mentioned as the women's main source of FP information (69.2%), while friends were mentioned by 24.6%, and the radio by 14.6% of respondents. Close relatives did not seem to be a very important source of information.
Interactions between providers and FP users
Table 1 summarises the level of provide/client interaction during the consultation. This includes the general environment of the consultation and the communication between provider and user. Around 70% of users said that the provider had informed them about the FP methods available at the health facility and about their mechanism of action including side effects. Almost two-thirds (63.5%) of the women said that they had received information from providers about the health advantages of using FP, both for the women themselves and their children.
Summary of the interactions between healthcare providers and family planning service users (n=671)
Responses ranged from 23.4% of users reporting that before the physical examination the provider had informed them of the procedures they could expect to experience, to 89.7% who said that the provider offered them a chair.
Waiting times for consultation and privacy
On average, women waited around 59.7 minutes in the healthcare facility before the consultation. The times varied from immediate access to waiting for more than 5 hours. The median waiting time varied by type of health facility. Health Posts generally reported waiting times considerably shorter than the other types of health facility. In general, the median waiting time was 30 minutes (interquartile range 10–90 minutes). When questioned about whether they felt their privacy had been respected, 85.8% of the women answered in the affirmative. Among the clients who felt that their privacy had not been respected, complaints included that they were not alone with the provider, the door was kept open during the consultation, and anyone could see them in the consultation room.
Women’s satisfaction
Table 2 summarises the level of satisfaction reported by women using FP services. Overall, 86% of women were satisfied with the services and only 2.6% were not satisfied at all. A waiting time in excess of 4 hours stands out as eliciting a report of ‘somewhat’ or ‘not satisfied’ from half the clients.
Satisfaction of women attending family planning services in Mozambique
As summarised in the logistic regression analysis in Table 3, women who had high levels of interaction with their providers were less likely to be dissatisfied than those who had a low level of interaction (OR=0.309, p=0.0292).
Odds ratio estimates for the general dissatisfaction of family planning service users in Mozambique
Unemployed women such as housewives (OR=0.361, p=0.0439) and women working in agriculture (OR=0.184, p=0.0009) were significantly more likely to be satisfied than employed women, but the difference between students or self-employed women and employed women was not statistically significant.
Women who waited 4+ hours were about 20 times more likely to be dissatisfied (p=0.0010) than those who waited <2 hours. No association was found between satisfaction and access to information or duration of contraceptive use, at least at the 5% level. Also, neither age nor type of health facility had a significant effect on women's satisfaction.
Discussion
This study explored the role that individual factors and service provision factors have on women's satisfaction with FP services. The study shows that the majority of women attending FP services in Mozambique were satisfied overall with the quality of services they received in the health facilities.
The results of this study indicated that the provider/client interaction played an important role in determining the level of woman's satisfaction. Similar results have been reported by other authors.17–19 Findings from the literature suggest that users of healthcare services tend to value their interaction with the provider, and this contributes significantly to the user's satisfaction.10 An evaluation of the barriers to sustained contraceptive use in Nepal concluded that detailed information given to users can have a significant and positive effect on the continuation of contraception as an alternative to group counselling.20 It also appears to be important that users be encouraged to ask questions about their own unique situations. In this study only 45.2% of women reported having the opportunity to ask questions of the provider. Usually patients give high importance to being able to ask questions and receive answers about their treatment.21
Waiting time has been reported as a very important contributing factor to client satisfaction regarding healthcare services.22–24 It has been suggested in other studies that waiting time not only has a negative impact on users but also on healthcare providers.25 In this study most of women spent an hour on average travelling to FP services. Consequently women are investing a total of 3 hours on average (including their trip home) in order to receive this service, while 17% of women waited more than 2 hours to see the provider and receive their FP methods. The odds of reporting dissatisfaction were 20 times higher among women who waited more than 4 hours to receive care, as compared with clients who had to wait <2 hours. However, waiting 2–4 hours was not significantly associated with dissatisfaction, suggesting that 4 hours of waiting is a threshold for patience and satisfaction. Innovative approaches to reducing the length of waiting times are desirable and are recommended for this setting.
Another important contributing factor to satisfaction was the woman's occupation. The minority of women who were self-employed or who were employed with a salary were more dissatisfied than women who were working in agriculture. Since women who were self-employed or employed with a salary tended to have higher levels of education than agricultural women, this suggests that there is an indirect association between education and levels of dissatisfaction with FP services.
An important programmatic finding was the proportion of women who had to switch their FP methods due to the lack of contraceptive availability at the healthcare facility. This highlights the importance of a functional logistic system in order to secure continuation of contraceptive use and ultimately contribute to client satisfaction. The current national FP policy in Mozambique indicates that women should receive at least 3–6 blister packs of pills at each follow-up consultation, depending on the distance to the nearest facility. In this study we found that clients on average only received 1.2 blister packs per consultation and 38.2% of women were dissatisfied with this low number of packs. The improvement of contraceptive stocking/logistics should be seen as a priority within the strategy of improving FP use in this setting.
The level of satisfaction among women using FP services in the health facilities may reflect the reality, or one could argue that this study has its limitations. Indeed human satisfaction is a complex concept that is related to a number of factors and expectations, to values of both individuals and society, and hence it can be very difficult to measure.26 Consequently, this type of survey can be affected by a courtesy bias resulting in users who are unwilling to criticise the system, particularly if the exit interview occurs within the health facility boundaries or nearby.27 Another source of possible selection bias is that the interviews cover only the users that visited the health facility, while those unsatisfied with the system may prefer not to use the health services in the public sector.
In conclusion, this study found high reported levels of overall satisfaction among women using FP services in Mozambique. However, it also identified clear issues requiring further intervention, namely: the need to improve the availability of contraceptives especially pills; the need to make the provider/woman interaction more informative and client-centered; and the need to resolve the issue of long waiting times. Addressing these bottlenecks may enhance client satisfaction and ultimately contribute to greater access and utilisation of FP services in Mozambique.
References
Footnotes
Competing interests None declared.
Ethics approval National Health Ethical Committee of Mozambique.
Provenance and peer review Not commissioned; externally peer reviewed.
Linked Articles
- Highlights from this issue


