Article Text
Abstract
Background Abortion in the second trimester may be performed surgically or medically. The objective of this systematic review was to examine the effectiveness, safety and acceptability/satisfaction of surgical compared with medical abortion of pregnancy between 13+0 and 23+6 weeks’ gestation for a new national guideline.
Methods We searched Embase, Medline and the Cochrane Library on 4 March 2019. We included randomised controlled trials (RCTs; any size) and non-randomised comparative studies with n≥100 in each arm, published in English from 1985. Risk-of-bias was assessed using the Cochrane Collaboration checklist for RCTs. Meta-analysis of risk ratios (RRs)
used the Mantel-Haenszel method. The quality of the evidence was assessed using GRADE.
Results Two RCTs (n=140) were included. ‘Incomplete abortion requiring surgical intervention’ was clinically significantly higher with medical than surgical methods (RR=4.58, 95% CI 1.07 to 19.64). ‘Abortion completed by the intended method’ was statistically, but not clinically, significantly lower after medical than surgical methods, but was marked by high between-study heterogeneity (RR=0.88, 95% CI 0.79 to 0.98). To the extent that ‘haemorrhage requiring transfusion/≥500 mL blood loss’, ‘uterine injury’, ‘cervical injury requiring repair’ and ‘infection reported within 1 month of abortion’ were reported, they did not differ significantly between methods. Depending on measurement method, ‘patient satisfaction/acceptability’ was either clinically significantly higher or comparable after surgical than medical methods. The quality of this evidence was limited by low event rates and attrition bias.
Conclusion Based on this evidence and consensus, women should be offered the choice of medical or surgical methods of abortion between 13+0 and 23+6 weeks’ gestation, unless not clinically appropriate.
- abortion
- family planning service provision
Statistics from Altmetric.com
Key messages
Abortion in the second trimester may be performed safely and effectively surgically using dilatation and evacuation or medically using mifepristone and misoprostol.
This systematic review examined the safety and effectiveness of surgical and medical abortion of pregnancy between 13+0 and 23+6 weeks’ gestation.
Based on this evidence and consensus, women should be offered the choice of medical or surgical methods of abortion between 13+0 and 23+6 weeks’ gestation.
Introduction
In the second trimester abortion may be performed surgically or by the administration of medications. Some women prefer surgical abortion because it is predictable and quick, and can be performed with a general anaesthetic or sedation. Others prefer medical abortion because it does not involve surgical instrumentation or anaesthesia.1–3
The recommended medical regimen in the second trimester is mifepristone followed 36–48 hours later by admission and repeated doses of the prostaglandin-analogue misoprostol.4 5 The median induction-to-abortion interval is 6–8 hours, with nulliparity, higher gestational age, and increasing maternal age associated with longer durations between the initiation of misoprostol and expulsion.6 The recommended method of surgical abortion in the second trimester is dilatation and evacuation (D&E).6 7 A D&E is characterised by preparation of the cervix using medications such as misoprostol or mifepristone or by insertion of absorptive natural or synthetic cervical tents (osmotic dilators) 3–24 hours preoperatively6 followed by removal of the fetus and placenta using specialised forceps. A D&E is an outpatient surgical procedure, may be performed with local anaesthesia, sedation or general anaesthesia, and takes about 10–15 min to complete.
Prior to current methods of medical abortion, previous medical alternatives to D&E involved saline, urea or prostaglandin F2-alpha. The comparative safety of D&E and medical abortion was first established by large cohort studies and case series conducted in the USA. Instillation of saline, urea or prostaglandin F2-alpha was demonstrated to carry a significantly higher risk of serious complications than D&E, including death.8 One randomised trial of D&E to instillation of prostaglandin F2-alpha confirmed that complications were less frequent with D&E, as were side effects.9 Modern medical abortion using mifepristone and misoprostol is safer and more effective, has much shorter induction-to-abortion intervals and is better tolerated than these outdated medical abortion procedures.10 In addition, in contrast to surgical D&E, the safety and success of the medical method depends on the medication and not on the skill of a surgeon. Moreover, studies have shown that both methods are safe and effective in the first trimester.3 11 12
Choice is an integral part of abortion care. Providing evidence-based information on the differences between methods is essential in helping a woman select the abortion method that is right for her.4 5 We performed a systematic review and compared the effectiveness, safety and acceptability of surgical and medical abortion of pregnancies between 13+0 and 23+6 weeks’ gestation in order to inform recommendations of method choices for a national guideline on abortion care for England.13
Methods
Eligibility criteria for study consideration
Randomised controlled trials (RCTs) of any size and non-randomised comparative studies with n≥100 in each arm, published in English from 1985 onwards were eligible for inclusion. A minimum number of 100 women in each arm was chosen because since allocation to treatment in such studies is non-random, the intervention groups tend to differ on a number of (baseline) characteristics that the analyses need to take into account in terms of adjustment. Balancing the need for covariate adjustment and a sample size that is appropriate for such analyses, alongside the desire not to miss any potentially relevant evidence of a reasonable quality, 100 was chosen as the minimum number of participants per arm where it was thought that such analyses can provide meaningful results, when also taking into account that meta-analysis of non-randomised studies is often not possible. The date 1985 was selected as mifepristone was not licensed for use prior to this date in any country. Eligible studies compared surgical (using D&E or vacuum aspiration) to medical (using mifepristone and misoprostol (any regimen)) abortion between 13+0 and 23+6 weeks' gestation, reporting any of the following outcomes: ‘incomplete abortion with the need for surgical intervention’, ‘haemorrhage requiring transfusion/>500 mL blood loss’, ‘patient satisfaction/acceptability’, ‘abortion completed by intended method’, ‘uterine injury (including rupture)’, ‘cervical injury requiring repair’, and ‘infection reported within 1 month of abortion’.
Information sources and search strategy
On 4 March 2019 we searched Embase Classic and Embase (1947–2019 March 01); Ovid MEDLINE(R) Epub Ahead-of-Print, In-Process & Other Non-Indexed Citations, Ovid MEDLINE(R) Daily and Ovid MEDLINE(R) (1946–2019 March 01); and Cochrane Database of Systematic Reviews (CDSR) and Cochrane Central Register of Controlled Trials (CENTRAL) on Cochrane Library via Wiley Online (March 2019; 3 of 12) using the search strategies detailed in online supplementary appendix S1. Once this search had been performed we only included records published from 1985 onwards in the final database. We also consulted experts in this field for any ongoing or missed trials.
Supplemental material
Study selection and data extraction
First, one author screened the titles and abstracts of the records identified by the computerised search, classifying them into ‘potentially relevant’ and ‘not relevant’. Second, the same author examined the full texts of the potentially relevant studies and classified them into ‘include’ and ‘exclude’. Third, the final list of included studies was confirmed by consensus between three of the authors: the author who had performed the screen and two authors who are experts in the field and familiar with the literature. One of the authors extracted the following data from each of the included studies: country, dates, aim, inclusion and exclusion criteria, baseline characteristics, surgical and medical abortion details and outcome data for each of the intervention groups. A further two of the authors performed spot checks of the extracted data.
Assessment of risk of bias
One author assessed the risk of bias in each of the studies using the Cochrane Collaboration quality checklist for RCTs.14 Selection bias and outcome reporting bias were assessed at study-level whereas performance bias, detection bias and attrition bias were assessed at outcome-level. We searched for, but did not find any, non-randomised comparative studies, which would have been assessed for risk of bias using the Newcastle-Ottowa scale for cohort studies.15
Data synthesis
All the outcomes were analysed as risk ratios (RRs). Meta-analyses were performed in Review Manager 5.316 using the Mantel-Haenszel method. Heterogeneity was assessed using the I2: if I2 was 0%–50%, a fixed effect model was used; if I2 was 51%–80%, a random effects model was used; and if I2 >80%, the RRs would not be pooled, but rather reported individually for each study. Subgroup analyses based on complex pre-existing medical conditions (none vs present) and whether the abortion was performed due to fetal anomaly (yes vs no) were planned. Whenever possible we aimed to conduct intention-to-treat analyses of the RCTs to preserve randomisation. Although we had not aimed to perform any sensitivity analyses, we performed a post hoc sensitivity analysis of a statistically, but not clinically (see below), significant result with an I2 of 48% by conducting a random effects analysis because we recognise that our I2 thresholds are relatively arbitrary and we wanted to further interrogate the robustness of a potentially weak result.
Quality of the evidence
The GRADE system was used to rate the quality of the evidence for each outcome using the GRADEprofiler Guideline Development Tool software.17 For a result to be considered clinically significant, a minimal important difference (MID; that is, effect size) between the intervention groups was defined as a statistically significant RR >1.25 or <0.8 for dichotomous outcomes and 0.5 times the SD of the control group for continuous outcomes apart from ‘haemorrhage requiring transfusion/>500 mL blood loss’, where simple statistical significance was also considered clinically significant due to the severity of this outcome. Imprecision was therefore present if the 95% CI of the RR crossed 0.8 and/or 1.25 or ±0.5 times the SD for all outcomes apart from ‘haemorrhage requiring transfusion/>500 mL blood loss’. As the MID for this outcome was statistical significance, the imprecision ratings were undertaken by using the optimum information size (OIS) so that if the total event rate ≥300, then the quality was not downgraded; if the event rate=150–299, then the quality was downgraded by one level; and if the event rate <150, then the quality was downgraded by two levels. When an outcome was reported as a median for which no MIDs are available, imprecision ratings were also undertaken by using the OIS so that if the total n≥400, then the quality was not downgraded; if the total n=200–399, then the quality was downgraded by one level; and if the total n<200, then the quality was downgraded by two levels.
'Incomplete abortion with the need for surgical intervention' was selected as a critical outcome due to the impact a second procedure will have on both the woman and on available resources. Although 'haemorrhage requiring transfusion/≥500 mL blood loss' is a relatively rare outcome, it was also selected as a critical outcome as it can be very serious when it occurs. The final critical outcome was 'patient satisfaction/acceptability' as abortion is an area where women are known to have strong preferences and providers wish to provide women with a service that meets their needs. Although 'cervical trauma', 'uterine perforation', and 'infection within 1 month of abortion' are rare in women undergoing abortion, they were included as important outcomes given the seriousness of such events and to allow for a balance of the benefits and harms of the different abortion methods to be assessed. 'Abortion completed by the intended method' was included as an important outcome to capture the failure rate of each abortion method as this also has implications for resource use and is likely to influence patient preference due to the need for a second visit if the chosen method fails.
Patient involvement
This systematic review was undertaken as part of the 2019 National Institute for Health and Care Excellence (NICE) guideline on ‘Abortion Care’,13 which was developed by a technical team at the National Guideline Alliance (NGA), based at the Royal College of Obstetricians and Gynaecologists (RCOG), and a guideline committee recruited specifically for this purpose. The guideline committee comprised a mix of clinical experts, commissioners and patient members, who collaboratively decided on the focus and specific parameters of the clinical question under consideration. Both the guideline scope and the draft guideline itself were also subject to public consultation before being finalised. During both consultations any organisation registering as a stakeholder could send in their comments, which the NGA/guideline committee took into account in the final versions of both the scope and guideline.
Results
Study selection
The search of all the databases identified 1732 records of which 1703 were excluded based on title/abstract and 29 were obtained for full-text review. Subsequently, 27/29 papers were excluded as they did not meet the inclusion criteria and two studies, both RCTs, were included (see online supplementary appendices S2–S3 for further details).18 19 We did not find any non-randomised studies meeting the inclusion criteria.
Study characteristics
The two included trials randomised a total of 140 women, 69 to medical abortion and 71 to surgical abortion (table 1, online supplementary appendix S4).
Summary of the characteristics of the included studies
Risk of bias of included studies
Both studies were at low risk of selection bias and selective reporting bias as they both had adequate generation of the randomisation list and allocation concealment, and reported the expected outcomes. Although both studies were also completely unblinded (women, healthcare staff, outcome assessors) we still considered the reported outcomes at low risk as they were either objective outcomes or only possible by the women knowing what they went through (‘patient satisfaction/acceptability’). One of the studies was also at low risk of attrition bias as it reported intention-to-treat analyses for all of the outcomes, however this study was stopped early due to slow recruitment, recruiting only 18 of a planned 60 women.18 The other study was considered at low risk for all reported outcomes (intention-to-treat analyses done for the majority of the outcomes), apart from ‘patient satisfaction/acceptability’, which was at high risk of attrition bias due to ≥50% missing data in each group19 (see also online supplementary appendix S4).
Synthesis of results
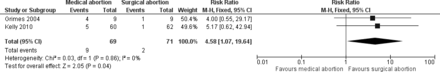
Meta-analyses were undertaken for all the outcomes with the exception of patient satisfaction/acceptability. The rate of ‘incomplete abortion requiring surgical intervention’ (table 2; figure 1) was clinically significantly higher and the rate of ‘abortion completed by the intended method’ (table 2; figure 2) was statistically, but not clinically, significantly lower after medical than after the surgical abortion of pregnancy. It is worth noting that in the latter case the between-study heterogeneity was high (I2=48%) and the use of a random-effects model, rather than fixed-effect model, for this analysis resulted in a statistically non-significant result (RR=0.83, 95% CI 0.57 to 1.22).
Summary of findings table
Incomplete abortion requiring surgical intervention. CI, confidence interval; df, degrees of freedom; M-H, Mantel-Haenszel method.
Abortion completed by the intended method. CI, confidence interval; df, degrees of freedom; M-H, Mantel-Haenszel method.
Grimes et al 18 did not directly report ‘haemorrhage requiring transfusion/≥500 mL blood loss’, ‘uterine injury including rupture’ or ‘cervical injury requiring repair’, but did report that no serious adverse events occurred. Kelly et al 19 found no significant differences in these outcomes between the medical and surgical abortion groups (table 2). None of the studies directly reported ‘infection reported within 1 month of abortion’, but infection was included in the definition of complications by Kelly et al,19 so presumably it was looked for, but not observed or reported by the authors; and Grimes et al 18 did report that three women had fever (>38°C) (table 2).
Surgical abortion was associated with clinically significantly higher or comparable patient satisfaction/acceptability compared with medical abortion, depending on how patient satisfaction/acceptability was measured: A clinically significantly higher rate of women would choose surgical abortion again than medical abortion;19 and a clinically significantly higher rate of women consider their experience of abortion worse than expected in the medical abortion group than in the surgical abortion group (table 2).19 There was no difference between surgical and medical abortion if patient satisfaction was measured as ratings of ‘satisfied with information/counselling pre-abortion’ at 2 weeks;19 ratings of ‘satisfied with care during the abortion’ at 2 weeks;19 ratings of satisfied with counselling/support post-abortion at 2 weeks;19 or as ratings on a scale from 1 (very satisfied) to 5 (very dissatisfied) at discharge (table 2).18 We had aimed to undertake subgroup analyses based on complex pre-existing medical conditions (none vs present) and whether the abortion was performed due to fetal anomaly (yes vs no), but the included studies did not report such data and therefore we were unable to perform these analyses.
Discussion
Main findings
The limited evidence that we found indicated that surgical abortion was either superior or comparable to medical abortion with mifepristone and misoprostol with respect to outcomes which were common enough to be evaluated in this systematic review. Although medical and surgical abortion did not differ significantly in terms of serious adverse events, very few adverse events were observed and the included studies were not powered to detect any difference in them between the abortion methods. Medical abortion was associated with a clinically significantly higher rate of an ‘incomplete procedure requiring surgical intervention’ and a statistically, but not clinically, significantly lower rate of ‘abortion completed by the intended method’ (although this finding did not hold up when using a random effects model). In addition, significantly more women would choose surgical abortion again if needed, and more women who had a medical abortion considered their experience worse than expected than those who had surgical abortion. Satisfaction with pre-, intra- or post-procedure care and overall satisfaction were not different between methods.
The quality of evidence for each of these outcomes ranged from very low (‘patient satisfaction/acceptability’), through low (‘haemorrhage requiring transfusion/>500 mL blood loss’, ‘uterine injury including rupture’, ‘cervical injury requiring repair’ and ‘infection reported within 1 month of abortion’) to moderate (‘incomplete abortion with the need for surgical intervention’ and ‘abortion completed by intended method’), and was mainly compromised by small event rates leading to imprecise results and, in the case of ‘patient satisfaction/acceptability’, by high attrition rates. Moreover, the studies did not include women having abortion of pregnancies ≥20+0 weeks’ gestation.
Strengths and limitations
Strengths of the study are that the research question was selected due to variation in practice in this area with a recognised need for guidance, and that the existing evidence base was examined in a systematic review using many of the well-established methods of the Cochrane Collaboration14 by experienced systematic reviewers within a long-standing guideline development framework with robust processes.20 However, the Cochrane Collaboration promotes the practice of two authors independently undertaking a number of the tasks associated with conducting a systematic review, such as dual sifting of the search and dual data extraction and bias appraisal. In this systematic review, only one author performed these tasks formally, but this was accompanied by a more informal process of dual sifting, and data extraction and bias assessment checking, through pre-existing knowledge of the evidence base and spot checks of some of the detailed study results by two of the other authors.
Limitations of the study include the few available studies, both of which were challenged with achieving recruitment goals. It is possible that there have been developments in service delivery of second-trimester medical and surgical abortion or in clinical protocols, including management of cervical dilation and pain, that might impact on the acceptability of either method now or in the future.21 22
Interpretation
When the committee that had been recruited to develop the 2019 NICE clinical guideline on ‘Abortion Care’13 considered the included evidence they noted that it was limited both in terms of number of included studies and their size, and that although the evidence favoured surgical over medical abortion for some of the outcomes (ie, ‘incomplete abortion requiring surgical intervention’ and ‘patient satisfaction/acceptability’), for other outcomes where the absolute risk was low (ie, ‘haemorrhage requiring transfusion/≥500 mL blood loss’, ‘uterine and cervical injury’ and ‘infection within 1 month of abortion’), the studies were not sufficiently powered to detect any between-group differences. The committee also noted that although the rate of abortions completed by the intended method did differ statically significantly between the methods, this difference was small, not clinically significant, marked by high between-study heterogeneity and did not hold up in a sensitivity analysis employing a random-effects model. Since evidence for the superiority of one method over another was either not available or did not allow differentiation between methods, a preference-sensitive care model that permitted choice dependent on how individuals value the risks and benefits of treatments was recommended. Moreover, the committee were aware that the included studies both had difficulties recruiting women to participate because this is an area of very strong patient preferences in terms of which method of abortion is wanted and of other studies demonstrating greater satisfaction with treatment if a woman was able to obtain the abortion method of her choice.2 23
When making the recommendations below, the guideline committee also took into account evidence systematically reviewed in connection with other areas of the guideline showing that women value a choice of procedure at all gestations (see Evidence reports A and B of the guideline13) and the fact that although the evidence comparing medical and surgical abortion before 13+0 weeks' gestation was not reviewed, studies have shown that both methods are safe and effective at this gestational age.3 11 12 Moreover, the committee agreed to extend the recommendations up to 23+6 weeks’ gestation despite the included evidence only covering up to 19+6 weeks’ gestation because in their experience and knowledge the safety and effectiveness of the methods does not increase markedly for one method over the other as gestational age advances and therefore the need for preference-sensitive decision-making remained relevant.
Many services in Britain only offer either surgical or medical abortion and it is anticipated that this recommendation will lead to development of services. There are also relatively few doctors trained to provide surgical abortion in the second trimester in the National Health Service (NHS), and most independent sector services do not provide inpatient medical abortion. In addition, many NHS services that offer medical abortion in the second trimester only do so for abortions in cases of fetal anomaly. To address these issues, greater collaboration may be needed between and across sectors to provide women with a choice of methods. Theatre teams in the NHS will need support if they are going to introduce a new service offering surgical abortion by D&E. Modern D&E practice uses ultrasound scanning during surgery, so scan machines need to be available in theatre and staff need to be able to undertake intraoperative scanning. In addition, surgeons will need training and a reasonable caseload of second-trimester abortions in order to attain and maintain their skills and low complication rates with D&E. Before services can start offering medical abortion, they need to ensure they have beds available and nursing or midwifery staff who are trained to care for women having medical abortion of pregnancy in the second trimester regardless of indication.
Conclusions
On the basis of this evidence and the clinical experience of the guideline committee recruited to develop the 2019 NICE guideline on ‘Abortion Care’,13 the committee agreed the following recommendations:
Offer a choice between medical or surgical abortion up to and including 23+6 weeks’ gestation1. If any methods would not be clinically appropriate, explain why.
To help women decide between medical and surgical abortion, see the NICE decision aid on choosing medical or surgical abortion: https://www.nice.org.uk/guidance/ng140/resources/patient-decision-aids-and-user-guides-6906582256.
Commissioners and providers should work together to ensure that women are promptly referred onwards if a service cannot provide an abortion after a specific gestational age or by the woman’s preferred method.
Additional educational resources
Lohr PA, Hayes JL, Gemzell-Danielsson K. Surgical versus medical methods for second trimester induced abortion. Cochrane Database Syst Rev 2008;1:CD006714. doi: 10.1002/14651858.CD006714.pub2.
Grossman D, Blanchard K, Blumenthal P. Complications after second trimester surgical and medical abortion. Reprod Health Matters 2008;16:173–82
British Pregnancy Advisory Service (BPAS) website: https://www.bpas.org.
Ethics statements
Acknowledgments
The authors would like to thank the National Institute for Health and Care Excellence (NICE), the National Guideline Alliance (NGA) and the Guideline Committee for the ‘Abortion Care’ NICE Guideline (2019).
References
Supplementary materials
Supplementary Data
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
Footnotes
Contributors PAL, SC, EH and MSH conceived and designed the review and wrote the protocol. EH devised and undertook the search strategy. MSH screened the search results and performed the data extraction and 'risk of bias' assessment of the included studies. MSH devised and performed the analysis strategy. PAL and SC interpreted the results. PAL, MSH, SC and EH wrote the first draft of different sections of the full review. All the authors critically revised the first draft of the review and approved the final version of the review.
Funding This article presents a systematic review undertaken as part of the 2019 National Institute for Health and Care Excellence (NICE) guideline on ‘Abortion Care’. This work was undertaken by the National Guideline Alliance (NGA) at the Royal College of Obstetricians and Gynaecologists (RCOG), which received funding from NICE. The funding body (NICE) did not play any direct role in the study design; the collection, analysis, and interpretation of data; in the writing of the report; or in the decision to submit the article for publication. The views expressed in this publication are those of the authors and not necessarily those of the NGA, RCOG or NICE. All researchers involved in this work were independent from the funding body at the time of completing this work.
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.
↵Surgical abortion can be performed shortly after 23+6 weeks’ gestation only if feticide is given at or before 23+6 weeks’ gestation, according to the 2019 clarification of the time limits in the Abortion Act.