Article Text
Abstract
Objective A weak and politicised COVID-19 pandemic response in the United States (US) that failed to prioritise sexual and reproductive health and rights (SRHR) overlaid longstanding SRHR inequities. In this study we investigated how COVID-19 affected SRHR service provision in the US during the first 6 months of the pandemic.
Methods We used a multiphase, three-part, mixed method approach incorporating: (1) a comprehensive review of state-by-state emergency response policies that mapped state-level actions to protect or suspend SRHR services including abortion, (2) a survey of SRHR service providers (n=40) in a sample of 10 states that either protected or suspended services and (3) in-depth interviews (n=15) with SRHR service providers and advocacy organisations.
Results Twenty-one states designated some or all SRHR services as essential and therefore exempt from emergency restrictions. Protections, however, varied by state and were not always comprehensive. Fourteen states acted to suspend abortion. Five cross-cutting themes surrounding COVID-19’s impact on SRHR services emerged across the survey and interviews: reductions in SRHR service provision; shifts in service utilisation; infrastructural impacts; the critical role of state and local governments; and exacerbation of SRHR inequities for certain groups.
Conclusions This study demonstrates serious disruptions to the provision of SRHR care that exacerbated existing SRHR inequities. The presence or absence of policy protections for SRHR services had critical implications for providers and patients. Policymakers and service providers must prioritise and integrate SRHR into emergency preparedness planning and implementation, with earmarked funding and tailored service delivery for historically oppressed groups.
- COVID-19
- reproductive health services
- reproductive rights
- sexual health
- health policy
- qualitative research
Data availability statement
The data that support the findings of this study are available on reasonable request from the corresponding author (MM). The data are not publicly available due to research ethics board restrictions.
This article is made freely available for use in accordance with BMJ’s website terms and conditions for the duration of the covid-19 pandemic or until otherwise determined by BMJ. You may use, download and print the article for any lawful, non-commercial purpose (including text and data mining) provided that all copyright notices and trade marks are retained.
https://bmj.com/coronavirus/usageStatistics from Altmetric.com
- COVID-19
- reproductive health services
- reproductive rights
- sexual health
- health policy
- qualitative research
Key messages
Protections for sexual and reproductive health and rights (SRHR) were either non-existent or piecemeal in the majority of US states’ COVID-19 emergency responses.
The COVID-19 response disrupted provision of, and access to, a range of SRHR services; these disruptions exacerbated inequities and will likely have long-term negative repercussions.
Future emergency responses should prioritise SRHR by linking comprehensive policy to infrastructural support for providers and tailored service delivery for disproportionately impacted groups.
Introduction
Structural determinants, including discriminatory policies, have driven reproductive health inequity in the United States (US).1 2 For example, the Trump administration’s “domestic gag rule” imposed abortion-related restrictions on Title X funding, putting 1.6 million patients at risk of losing affordable reproductive healthcare3 and disproportionately impacting historically oppressed groups or people of colour, immigrants, people with low income, and uninsured or underinsured individuals.4 Additionally, anti-immigration policies like the public charge rule render immigrants ineligible for Permanent Resident Cards if they use public benefits, reducing immigrant families’ access to health services.2
The coronavirus disease 2019 (COVID-19) pandemic further threatened the sexual and reproductive health and rights (SRHR) of women, girls and historically oppressed populations.5 A weak and politicised COVID-19 response in the US6 and lack of attention to SRHR converged with policy responses that heightened racial and economic disparities. Response policies also deliberately subverted SRHR, with government officials using pandemic lockdowns to further restrict abortion.7 8
Recent studies document COVID-19’s impact on women’s SRHR experiences in the US, with a particular focus on fertility, childbearing preferences and contraceptive access9–11; however, less is known about the pandemic’s impact on providers and the provision of SRHR care, including abortion, contraception, sexually transmitted infection (STI)/HIV care, maternal health and delivery, and community outreach. Thus, this study’s aim was to assess how COVID-19 affected SRHR service provision during the first 6 months of the pandemic. The study used a multiphase, mixed method approach that included policy mapping, a provider survey, and provider and advocate interviews to understand barriers to SRHR policy and services in the COVID-19 era, and to identify strategies to prioritise SRHR during future large-scale emergencies.
Methods
This was a multiphase, three-part, mixed method study incorporating: (1) a comprehensive review of state-by-state emergency response policies, (2) a survey of SRHR service providers and (3) in-depth interviews with SRHR providers and advocacy organisations. A preliminary policy scan informed the sample selection for the survey (exploratory sequential design), and then the comprehensive policy review, survey and interviews were conducted concurrently (convergent parallel design).12
The policy analysis identified SRHR protections and restrictions adopted by states in their COVID-19 responses. We reviewed emergency orders and official guidance issued during the spring and summer of 2020 related to non-essential business closures, essential service designations, and mobility restrictions, including stay-at-home orders. We cross-checked our analyses with other COVID-19 state policy reviews.13–15 Our review mapped state-level actions to suspend abortion and to protect SRHR services (abortion, contraception, STI/HIV care, maternal health and delivery, and community outreach). We defined action to suspend abortion as any statewide policy, order or official guidance limiting abortion provision. Action to protect SRHR services is defined as any statewide action to designate any SRHR service essential.
Ten states were selected as a purposive survey sample (online supplemental appendix 1). We sought diversity in geographic region, demographics and SRHR policy landscape (as identified in a preliminary policy scan), and early COVID-19 hot spots or epicentres of racial justice movements. Public and private SRHR providers were identified, accounting for rural, urban and suburban representation. Providers included family planning centres, abortion clinics, sexual health clinics, maternal health programmes and adolescent programmes. The email-distributed survey included 39 questions about COVID-19’s impact on service provision and funding and the general state of SRHR services in the US. Univariate data analyses, conducted by one author in STATA version 16 (StataCorp), indicated trends in service provision and funding.
Supplemental material
Semi-structured interviews were conducted with 15 SRHR organisations, with targeted outreach to organisations in the 10-state survey sample serving historically oppressed groups. Topics included shifts in service availability and modality, facilitators and inhibitors to continued operations, and government responses to SRHR needs during the pandemic. Interviews lasting 45–60 minutes were conducted over Zoom or telephone according to participant preference, and were recorded and transcribed. Two authors independently coded transcripts by hand for content and performed thematic analysis. Integration of study findings was achieved through regular meetings where team members interacted about emerging qualitative and quantitative results and achieved consensus.12 16 Per study procedures approved by institutional review board, informed consent was obtained for all participants, and data were protected and stored.
Patient and public involvement
Patients and/or the public were not involved in the design, conduct, reporting or dissemination plans of this research.
Results
Policy review
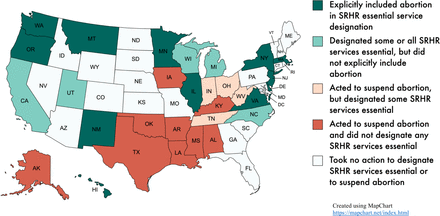
In March and April 2020, all states issued COVID-19 emergency declarations, 45 states closed “non-essential businesses” and 44 issued mobility restrictions.14 Twenty-one states designated some or all SRHR services essential (figure 1) and exempt from emergency restrictions.13 Precise protections varied by state, including essential designations for “reproductive health services”, “pregnancy-related procedures”, “obstetrics-gynaecology” and “all healthcare services”.13 Protections were not always comprehensive. Some protections only applied to services provided under Medicaid.17 Only 12 states explicitly protected abortion, for example, by specifically stating abortion is not considered a non-essential or elective procedure,18 exempting all reproductive health providers from stay-at-home orders19 or designating the “full suite of family planning services” as non-elective procedures.20
Sexual and reproductive health and rights (SRHR) essential service designations and actions to suspend abortion by state
Fourteen states acted to suspend abortion by excluding it from the list of essential or non-elective services allowed to continue during shutdowns.7 14 15 This included four states – Indiana, Ohio, Tennessee and West Virginia – that designated some SRHR services essential while also acting to suspend abortion (online supplemental appendix 2).
Survey of service providers
A total of 97 respondents completed the survey (table 1). Of those respondents, 56% worked in gender-based violence (GBV), 18% in SRHR and 24% in both GBV and SRHR. Thus, 40 respondents were able to provide information on SRHR impacts across the 10 sampled states. Nearly all (99%) agreed their work had been impacted by COVID-19. Five cross-cutting themes surrounding COVID-19’s impact on SRHR services emerged across the survey and interview findings: reductions in SRHR service provision; shifts in service utilisation; infrastructural impacts; the critical role of state and local governments; and exacerbation of SRHR inequities for certain groups.
Descriptive characteristics, sexual and reproductive health and rights (SRHR) service providers survey, United States, 2020
Respondents reported their SRHR work stopped or was reduced due to lockdowns/movement restrictions early in the pandemic (53%). Others reported their work was deemed non-essential and thus was forced to stop (20%). Findings also indicate reduced service demand (25%) and simultaneously a strain on staff with increased workload to support the emergency response in addition to regular work (25%). The majority of respondents (83%) reported continuing service delivery using technology and other strategies. Survey respondents also identified groups lacking services including adolescents (20%), women with disabilities (18%), black, indigenous and people of colour (30%), migrants, refugees and displaced populations (28%) and lesbian, gay, bisexual, trans and queer (LGBTQ) individuals (20%).
Interviews with service providers and advocates
Fifteen organisations working on a range of SRHR focus areas in 15 states participated in interviews (table 2). The majority of interviewees worked for direct service organisations (73%) and held leadership roles (73%).
Selected characteristics of sexual and reproductive health and rights (SRHR) service provider and advocate interviewees, United States, 2020 (n=15)
Five themes emerged from the interviews (box 1).
Themes and quotations from semi-structured interviews with sexual and reproductive health and rights (SRHR) service providers and advocates, United States, 2020 (n=15)
Reductions in SRHR service provision
“All the [abortion] clinics in [state] were closed. Toward the end of March some clinics were doing medical abortions, but they weren’t really advertising that because they weren’t sure if they were against the order. So this pushed a lot of our clients to have to wait.” [R12, Abortion/Community Outreach, South]
“We shifted from doing routine [sexually transmitted infection (STI)/HIV] screenings to just triaging individuals that needed to be treated based on signs and symptoms.” [R5, STI/HIV Care, Midwest]
“We used to go to meetings, tabling events […] [Now] there is no ‘out in the community’. […] and people who could benefit from information or access, they’re not people who linger online.” [R1, Abortion/Contraceptive Services/Community Outreach, South]
“It’s been more challenging to provide [teen education] sessions due to privacy, access to phones, them answering the calls and accepting to see a health educator, and so on.” [R2, Community Outreach, Northeast]
Shifts in service utilisation
“People are looking for something long-term to kind of wait this whole thing out. So we’ve seen a lot more interest, but not the funding for, implants, IUDs [intrauterine devices].” [R1, Abortion/Contraceptive Services/Community Outreach, South]
“There was a drop in referrals for us because everyone was scrambling to figure out what to do […] and I was getting really concerned because people need doulas now more than ever.” [R6, Maternal Health/Community Outreach, Northeast]
“[Young people] were not able to find any excuse to get out of the house, to go to the clinic, to go to the courthouse, or to get the abortion. So we did see a decrease in people that actually followed through the whole process.” [R12, Abortion/Community Outreach, South]
“Even increasing [STI/HIV testing hours], we’re still not seeing the numbers. We’ve also noticed a drop in our PrEP [pre-exposure prophylaxis] clients. Usually […] we get a lot of funnelling in from our testing programme.” [R9, STI/HIV Care/Community Outreach, West]
Infrastructural impacts
“COVID-19 fractured our team in some ways […] We’re processing isolated.” [R9, STI/HIV Care/Community Outreach, West]
“The two biggest prisons have massive [virus] outbreaks. Even if we could get access, I don’t think it would be safe or ethical for me to encourage or allow my staff to go back inside.” [R16, Maternal Health, Midwest/South]
“In saying doulas need to be allowed in labour and delivery, they were basically considered essential workers, yet weren't being provided with PPE [personal protective equipment] like essential workers.” [R6, Maternal Health/Community Outreach, Northeast]
“Our supply chain systems fell apart because the UPS [United Parcel Service] shut down, so things were much more expensive. We would order things, never get them […] General cost of operations basically doubled.” [R15, Maternal Health, South]
“When COVID-19 hit, the Governor’s budget and revenue generated in the state through taxes […] all the things that feed into our coffers virtually dried up.” [R14, Abortion/Contraceptive Services/STI/HIV Care/Community Outreach, Northeast]
“Our work is so intersectional, and the criminal justice system and justice-involved people are so stigmatised that some of the very big funders […] will say things that are inappropriate, biased. They’ll say ‘We don’t see people in prison as part of our community, and we only fund community projects’.” [R16, Maternal Health, Midwest/South]
Critical role of state and local governments
“The Governor, luckily, put in quarantine for anybody travelling into the state, but made a little exception for people travelling for healthcare […] I think our Governor is pretty good on reproductive health and had us in mind when making that caveat.” [R20, Abortion, West]
“The Governor’s been incredibly responsive from a public health standpoint. We’re actually flattening. In early August, we began opening up our practice to more in-office preventive visits.” [R14, Abortion/Contraceptive Services/STI/HIV Care/Community Outreach, Northeast]
“Normally, I’d be at the [US state] Capitol at least once a week. None of us went a single day this session. I didn't feel comfortable going. There was no mask requirement.” [R13, Advocacy, South]
Exacerbation of SRHR inequities for historically oppressed groups
“Communities of colour and rural communities, for us getting the word out about our services is a challenge in itself. And black and brown and indigenous communities, I think all of the barriers to care they were facing before have been exacerbated overall.” [R23, Abortion/Contraceptive Services/STI/HIV Care/Community Outreach, Midwest]
“As an adult if I were to get birth control [by telehealth], it would be easier […] If you are under 18, you have to go to a specific Title X clinic, that clinic is probably not offering telehealth for birth control appointments, especially for people who never had a visit. So, that’s making it even harder.” [R12, Abortion/Community Outreach, South]
Reductions in SRHR service provision
Respondents described significant operational disruptions resulting in reduced service provision, shifts in healthcare delivery, and diminished service quality. STI/HIV clinics reduced hours, eliminated walk-in testing, and prioritised urgent cases. Doulas were forced to offer prenatal and labour support remotely, and direct outreach for doula and family planning services ceased. Abortion providers reported challenges implementing social distancing protocols (eg, staggering appointments and reducing waiting room capacity), obtaining personal protective equipment (PPE), finding local clinicians, and navigating abortion bans and travel restrictions. While some family planning providers moved up appointments prior to lockdowns, extended prescriptions, and expanded telehealth, the shift to telehealth was described as “extremely disruptive” when infrastructure was lacking. As schools and community-based organisations closed, adolescent sexual health education moved online, which proved difficult to implement due to privacy and participant engagement. Advocacy was impacted by shortened legislative sessions and deprioritised by policymakers; one interviewee described feeling “perpetually on hold”.
Shifts in service utilisation
Respondents noted shifts in demand for, and access to, SRHR services. Doula referrals initially plummeted because “everyone was scrambling to figure out what to do”. Abortion bans under state emergency orders blocked or delayed abortion access. Stay-at-home orders restricted adolescents’ mobility, limiting their access to SRHR services. STI/HIV clinics reported reduced testing uptake in the spring. While one respondent saw a rebound – partly due to a backlog following a pause in routine screenings – another said numbers remained low despite extending operating hours, resulting in fewer pre-exposure prophylaxis (PrEP) referrals. Declines in family planning service volume were reported, possibly due to clinics triaging patients towards telehealth, people losing health insurance, or fear of coronavirus infection. In some cases, demand for SRHR services increased (eg, requests for long-acting contraceptives). Home birth requests were described as “skyrocketing”, with not enough midwives to meet the need.
Infrastructural impacts
Service providers struggled to adapt organisational infrastructure to pandemic-related stressors. Staffing emerged as a salient concern with a combination of increased workloads, frustration with ever-changing protocols, lack of childcare, social isolation, grief and fear. Respondents worried about staff exposure to coronavirus, particularly respondents serving incarcerated populations given their disproportionate COVID-19 exposure. Respondents also discussed supply chain disruptions from resource reallocation and scarcity. Supply-related cost increases were coupled with decreased revenue streams. Some organisations cancelled or moved fundraising events online, reducing ability to meet fundraising goals. Lower patient volumes also translated to less revenue. The pandemic created uncertainty about future funding, including concerns about state budget cuts and private funding, noting foundation priorities and grant timelines did not meet their needs.
Critical role of state and local governments
Many respondents mentioned state and local government officials when asked about key factors that facilitated continued operations. Abortion providers cited exemptions from state emergency orders as critical. Others described effective government-led activities, such as frequent communication of data-driven recommendations which facilitated reopening, or county-level coordination which streamlined PPE distribution. Some respondents noted states’ pre-pandemic policy landscapes, especially flexibility around Medicaid telehealth reimbursement, helped mitigate COVID-19’s impact on provision of, and access to, SRHR services. In other cases, state and local governments inhibited operations. For example, failure to impose a mask mandate kept one respondent from continuing in-person advocacy at the [US state] Capitol.
Exacerbation of SRHR inequities for historically oppressed groups
Respondents stated that access to SRHR services was unequal. They identified several historically oppressed groups with unmet SRHR needs prior to the pandemic – including those with limited English proficiency, immigrants, rural populations, black, indigenous and people of colour, people with low income, and LGBTQ individuals – and emphasised that gaps in access were widening. Youth were cited as experiencing disproportionate SRHR impacts due to COVID-19, in part because school closures limited adolescents’ mobility and telehealth services did not always reach adolescents.
Discussion
Despite some evidence that the pandemic response has shaped SRHR services in the US8 21 22 and the experiences of people seeking SRHR services,10 11 23 few studies consider the response’s impact on SRHR providers across a range of services. This multiphase, mixed method study offers valuable insights into how the COVID-19 policy response shaped SRHR service provision by situating providers’ experiences within the context of protective or restrictive state policies. The integrated policy review, survey and interview results demonstrate that the majority of states failed to protect SRHR in their COVID-19 responses and providers were forced to close or find innovative ways to continue operating amid increasing restrictions and diminishing resources.
In alignment with existing policy scans documenting states’ actions regarding SRHR during the pandemic,13 14 our study suggests less than half of US states established protections for SRHR services during the pandemic, many of which were not comprehensive. Emergency stay-at-home orders and definitions of essential determined which services were available and to whom. SRHR providers were forced to limit in-person and walk-in visits and deprioritise preventive services. Providers’ attention was diverted from routine service delivery as they reworked how services were provided and funded within changing restrictions. Abortion providers faced unique challenges and at times were forced to cancel or delay services, especially in states that suspended abortion or implemented travel restrictions. This supports other research anticipating additional barriers to provision of, and access to, later abortion services during the pandemic.8 Policymakers’ failure to anticipate and respond to these patterns reflects an overwhelming disregard for SRHR.
Both survey and interview results demonstrate that these policies – or lack thereof – had critical implications for providers where protections for SRHR services were non-existent or piecemeal, creating confusion, closures and delays. Where protections were in place, providers faced fewer barriers. However, challenges related to staffing, supply shortages, outreach, telehealth capacity, increased costs, and diminished funding remained, underscoring a need to link policy to implementation. These findings align with prior research indicating restrictions on public funding for family planning programmes reduce service availability and participation24 and research in Europe showing abortion regulation responses to COVID-19 led to fragmented SRHR care.25
These policy implications are particularly grave for historically oppressed groups. Providers highlighted that these groups had trouble accessing SRHR services. Provider and advocate accounts of barriers for adolescents, black, indigenous and people of colour, immigrants, incarcerated populations and LGBTQ individuals align with other research anticipating greater vulnerability during COVID-19.2 23 26 Findings also align with a study showing low-income women, Hispanic and black women, and queer women were most likely to experience pandemic-induced delays in accessing contraception and SRHR services.10 This underscores the urgency of addressing policy impacts, as disruptions in care can have health, social and economic consequences for historically oppressed populations.
This study is not without limitations. States were purposively selected based on social and political factors relevant to SRHR care to explore the role these factors played in service provision. Therefore, the findings are only representative of the 10 included states. Further, we oversampled organisations serving historically oppressed populations with the intent of capturing overlooked perspectives. This targeted approach should be considered for generalisability of the study findings.
The immediate impacts of COVID-19 on SRHR service provision are likely to have long-term repercussions. Decreases in SRHR services, family planning appointments, and education and outreach will shape SRHR service demand and reproductive outcomes into the future. Reduced contraceptive access increases risk for unintended pregnancies,27 and delaying annual visits means cancers may go undetected.28 Decreased STI/HIV screening may lead to undetected infections and reduced PrEP referrals. Risks due to limited access to doulas and other maternal health services are established, and are particularly concerning in the US, which has high black maternal and infant mortality.29
SRHR should be prioritised and integrated into emergency preparedness planning and implementation. State-level policy must be explicit and unambiguous in protecting the full suite of SRHR services, including abortion. For historically oppressed groups, it is imperative to expand health insurance coverage, eliminate discriminatory policies, earmark funding, and tailor SRHR service delivery. Since telehealth helps address in-person visit barriers,30 states should support providers’ telehealth capacity and strengthen reimbursement mechanisms, while also addressing the digital divide.
This study reveals a lack of prioritisation of SRHR in the US COVID-19 response at the expense of SRHR service providers and historically oppressed groups. The pandemic response has magnified funding uncertainties, exacerbated pre-existing disparities, and further fragmented the provision of SRHR services in the US. Future policies, emergencies and pandemics must centre SRHR in response procedures and ensure immediate, comprehensive protections for SRHR service provision to reduce disparities.
Data availability statement
The data that support the findings of this study are available on reasonable request from the corresponding author (MM). The data are not publicly available due to research ethics board restrictions.
Ethics statements
Patient consent for publication
Ethics approval
The study protocol was approved by the Columbia University Irving Medical Centre Institutional Review Board (protocol #AAAS9211).
Acknowledgments
The authors would like to thank the Ford Foundation for funding this research and the survey and interview participants for generously sharing their time, experiences and insights.
Supplementary materials
Supplementary Data
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
Footnotes
Contributors TM (study Principal Investigator) conceived the study and secured funding. GS and TM developed study instruments with input from MM, JO and CB. MM and JO collected the data, and MM, GS and JO conducted the analyses. All authors (MM, GS, JO, CB and TM) contributed to the interpretation of the data. MM, GS and JO created the first draft of the manuscript, and GS, CB and TM offered critical revision. All authors read and approved the final manuscript.
Funding This study was supported by the Ford Foundation (grant #133189; TM, Principal Investigator).
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.